What you need to know about living or communicating with a person with Aphasia
You may have heard about aphasia before, or you are only just learning about it because your loved one has been diagnosed with it.
Aphasia is a language disorder that occurs when there is some type of damage to the brain; this could be due to head trauma, stroke, dementia for example. Aphasia results in difficulties in understanding what someone is saying, speaking, reading, and writing. The severity and type of difficulties will depend on the size and location of the brain damage.
You can read more in our previous blog ‘What is Aphasia?’.
Living with aphasia is very difficult – can you imagine how frustrating it would be to be able to form full sentences in your mind and only be able to get a word or two out. Or you can recall lots of stories and memories about your loved ones but have trouble saying their names.
That is the reality for people living with aphasia. With this in mind – the two most important things for living or communicating with someone with aphasia is to exercise patience and empathy.
It is important to remember.
- Aphasia is not a reflection of a person’s intelligence; there is a difference between not being able to provide an answer and not knowing an answer. You may need to ask if they have an answer and just can’t get it across.
- A person with aphasia (or anyone for that matter) might need a different approach to get the same result. If you are working with someone with aphasia you might need to assist them in finding an easier way for them to perform a task.
- When a person with aphasia is talking – listen patiently, the speaker may have difficulty finding the words or they may stumble, this is okay – be patient. Focus on what the person says, not what they haven’t been able to say.
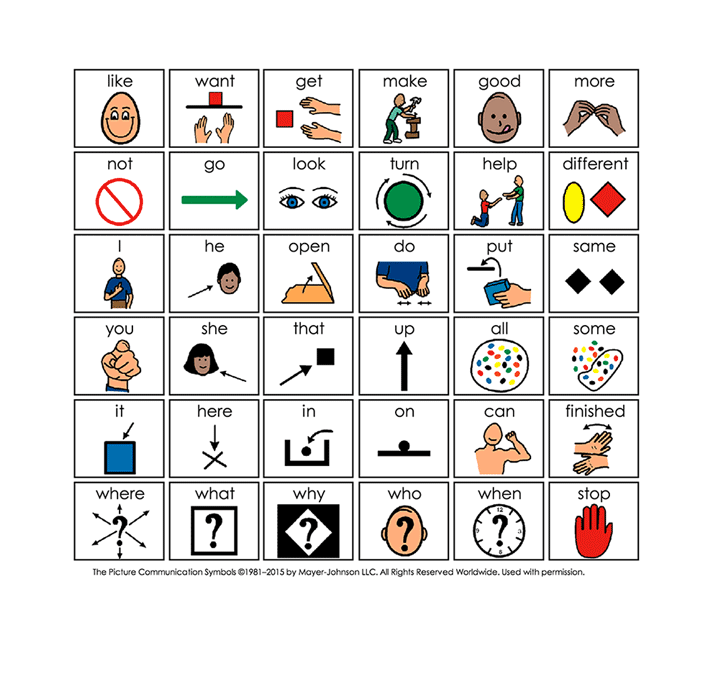
- Simple is best – keep distractions and noise to a minimum. Use adult language but keep it simple and concise. Break down lengthy instructions. Use gestures, pictures, or other means to help support your communication.
- Just because a person with aphasia may have difficulties, does not mean they should avoid all communication. Keep the person involved. Involve them as much as you can with decision making but avoid burdening them with day-to-day details.
- Not everyone with aphasia is the same, just like every human – they are individuals with their own needs and wishes, so support will differ.
Tips for communicating with someone with Aphasia

- Make sure that you have their attention before you start talking. This may include getting them to face you and getting their eye contact.
- Minimise background noise where possible e.g. Turn the TV down, move to a quieter room.
- Pay attention to the person’s body language and gestures they use.
- Keep your voice at a normal level unless I ask otherwise.
- Keep communication simple but don’t ‘talk down to them.
- Use short sentences. Repeat keywords if needed.
- Slow down.
- Give them time to listen, process and respond. This is likely to take a little longer than usual, but do not try and finish sentences for them.
- Try using different modalities of communication – drawings, gestures, writing, facial expressions. It may be easier to understand than words at times.
- Ask them to try another way e.g. drawing, pointing, or writing if they are having trouble.
- Ask ‘yes’ or ‘no’ questions.
- Let them make a mistake – this is okay.
- Let them try to do things for themselves. They may need multiple attempts, help when asked.
Practice kindness – and reach out for support where needed. Your speech pathologist is here to help you and your loved one navigate through this tricky time.
There are some fantastic resources out there – here are some below.